Concurrent disorders are mental health challenges and substance use disorders that happen at the same time. Depression and alcohol dependence is one example of a concurrent disorder.
What is substance use?
Substance use refers to the use of alcohol or drugs, including substances like nicotine, caffeine, prescription drugs, and illegal drugs. Substances make us see, think, feel and behave differently than we usually do.
Some youth may start to use substances to help them cope with stress, anxiety or depression. There may be conflict at home, school or among their peers. They may be questioning their sexuality and gender. Some children and youth may naturally be more likely to take risks than others or may hold some beliefs that influence their behaviour. For example, they may begin using substances such as vaping nicotine because they think it will lower their appetite or help them will fit in with peers.
How substance use can become a problem
Some people can use substances without it being a problem. However, it is recommended not to use any substances while the brain is still growing. Substance use in a growing brain can interfere with learning, memory, and increase your risk of developing a substance use disorder as an adult.
These are the stages of substance use:
It is normal for youth to experiment, but substance use can become a problem if it starts to interfere with daily life and mental health. It’s important to recognize the different stages of substance use and pay attention to your child’s mental health.
These are the stages of substance use:
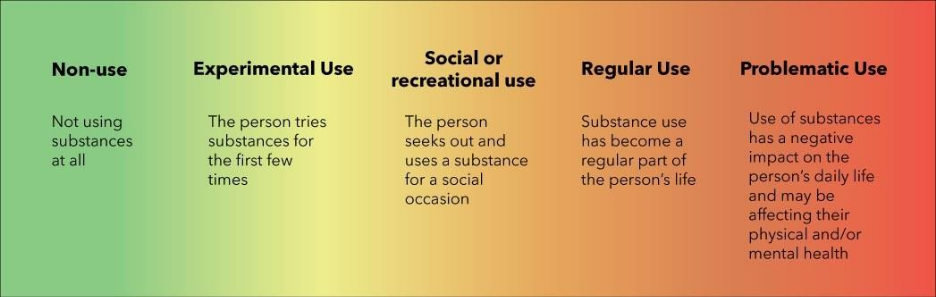
Problematic substance use means alcohol or other drug use is linked to problems such as:
Health problems like diabetes or mental health concerns, such as psychosis
Problems with friends, family or people at school
Risky behaviour:
Taking a lot of substances all at once
Mixing substances (poly drug use), like drinking alcohol and taking sleeping pills at the same time
Using substances while riding an electric scooter or cycling
Using substances and going to work or school
What is a mental health challenge?
A mental health challenge is a condition that affects the way you think, feel and behave. There are many kinds of mental health challenges, for example:
How are substance use problems and mental illnesses connected?
There are four general ways that mental health challenges and substance use problems go together:
A mental health challenge comes first. Example: A young person is experiencing a mental health challenge and uses substances like alcohol or other drugs to help them deal with troubling symptoms.
A mental health challenge and a substance use disorder are triggered by the same event. For example, someone is in a very serious car accident and uses opioids to cope with nightmares and flashbacks.
The problems start separately. Example: A young person was diagnosed with separation anxiety in elementary school. There is a family history of anxiety disorders. In high school, they go to a party and are introduced to alcohol. They start drinking daily at school and this leads to an alcohol use disorder.
Substance use and mental health challenges are also connected when they're being treated:
Some substances stop medications from working properly, so symptoms of a mental health challenge become worse.
Some mental health challenges such as psychosis might make it harder to go through some substance use treatments.
Some mental health challenges can get worse if someone stops or cuts back their substance use without proper help.
Some people don't take their medication when they're using a substance, and this makes symptoms of a mental health challenge worse.
When one problem gets worse it can make the other problem worse. For example, drinking alcohol can make symptoms of depression worse.
When a mental health challenge is treated, the substance use may decrease.
For these and other reasons, it's important to take care of both concerns at the same time.



